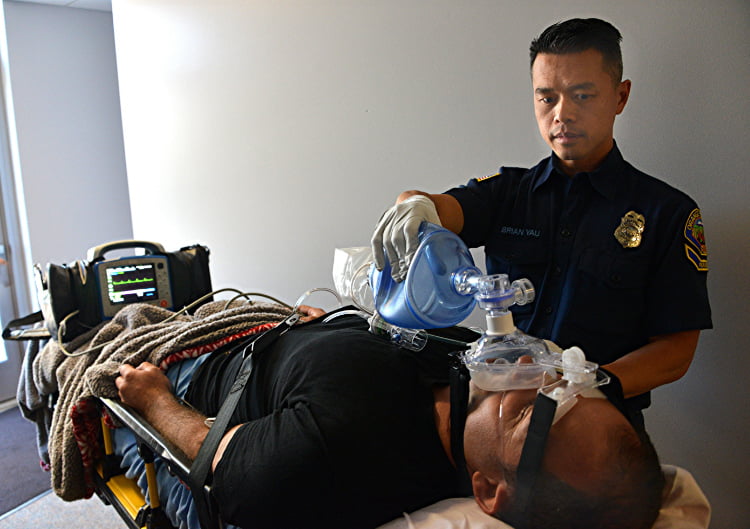
High-risk, low-frequency procedures such as CPAP leave little room for error. (Photo/Rick McClure)
Preventable injuries resulting from medical errors are a leading cause of death among Americans. Despite extensive study in hospitals and outpatient care facilities, and concerted error reduction efforts, their occurrence remains remarkably high.1 At least two out of every three major medical errors result from miscommunication between providers, often during handoffs of patient care from one provider to another.2 The paucity of prehospital medical error research leaves us unable to estimate the number of patients harmed, but there is no reason to believe they occur any less frequently. In fact, lack of resources available in hospitals such as computerized medication administration systems, online references and instant access to multiple colleagues suggests that EMS may make more errors and cause more harm than hospitals. Suffice it to say that lifesaving procedures like CPAP (Continuous Positive Airway Pressure) pose tremendous risk to patients if miscommunications occur during handoffs. The focus of this article is on reducing these errors.
We have all delivered patients to emergency departments (ED) at one time or another when it seemed abundantly clear that the nurse or team we were addressing was either disinterested or not paying attention to our report. Before we reach the ED, many of us hand off our patients to others. This might be from a BLS to an ALS crew, from first responders to a transport ambulance crew or perhaps from scene personnel to an air medical crew. Like the occasional bumpy ED transition, handoffs in the field do not always go smoothly. Problematic exchanges are a breeding ground for miscommunication, each with potential to result in patient harm. To safely transition patient care, everyone involved should have a practiced routine and be acutely aware of what needs to be communicated.
Use of CPAP is both an art and science (see Successfully Selling CPAP). As such, conveying the nuances of how you successfully treated an acutely dyspneic patient with CPAP will help receiving providers continue your excellent care. Early notification is the most essential element of a CPAP handoff. Typically, prehospital providers initiate CPAP with a disposable device and these may require a standard flowmeter, or a high flow (40-60 psi) outlet. Advising an incoming unit well before their arrival that you are using CPAP and the type of oxygen connection needed will help them prepare to transition care. In the case of a receiving hospital, it may be necessary for the emergency department to summon a respiratory therapist who, in turn, will need to set up a ventilator or BiPAP machine. Early notification provides opportunity for readiness prior to arrival.
Second to early notification is conveying the reason why you chose to use CPAP or, in other words, the indication for CPAP. The time to peak effect of CPAP is very condition dependent (see The Evidence for Prehospital CPAP). Acute pulmonary edema (APE) responds immediately to CPAP; patients would quite likely be considerably improved at handoff, regardless of how quickly the transfer occurs.3 They are however, quite likely to rapidly deteriorate with any interruption in pressures or flow (one reason why many EMS protocols prefer intravenous instead of sublingual nitro for acute pulmonary edema).4 Patients with acute asthma or COPD exacerbations improve more slowly with CPAP and tend to tolerate breaks in their CPAP circuit better than APE patients. This is quite helpful knowledge when assuming patient care, as are pre- and post-CPAP assessment findings, pressures and any other pertinent settings. Ideally, you want to paint a picture during handoff of exactly how the patient appeared prior to initiating CPAP, how you measured improvement, what adjustments you made, and exactly how their current status compares to what you observed on arrival.
The subtle nuances that categorize as the ‘art’ of using CPAP can also be very helpful to convey in report. These include the estimate amount of mask leak, calming techniques you found effective for gaining patient cooperation with CPAP, EtCO2 measurements used to evaluate effectiveness, and respiratory rate and perceived depth.
Keep in mind that tired providers make nearly twice as many errors than those who are well rested5. Be particularly vigilant when you feel exhausted or find yourself doing a handoff at the end of a tour; you may not realize that miscommunications have occurred. Checklists help to cover your bases, keep you focused on what’s important, and assure you cover essential information.
Recognizing that the majority of medical errors happen during transitioning care from one provider to another help to focus attention on reducing this common cause of patient harm. High-risk, low-frequency procedures such as CPAP leave little room for error. These should serve as a flag for all of us to focus on detail, communicate clearly, and advocate for those we are called to care for.
References
- Landrigan CP, Parry GJ, Bones CB, Hackbarth AD, Goldmann DA, Sharek PJ. Temporal trends in rates of patient harm resulting from medical care. N Engl J Med 2010;363:2124-2134.
- Starmer AJ, Spector ND, Srivastava R, West DC, Rosenbluth G, et al., for the I-PASS Study Group. Changes in Medical Errors after Implementation of a Handoff Program. N Engl J Med 2014; 371:1803-1812. On-line, available at nejm.org/doi/full/10.1056/NEJMsa1405556.
- Weng CL, Zhao YT, Liu QH, et al. Meta-analysis: noninvasive ventilation in acute cardiogenic pulmonary edema. Ann Intern Med. 2010;152:590-600.
- Barach AL, Martin J, Eckman M. Positive pressure respiration and its application to the treatment of acute pulmonary edema. Ann Intern Med 1938;12:754-95.
- Scott LD, Rogers AE, Hwang WT, Zhang Y. Effects of critical care nurses’ work hours on vigilance and patients’ safety. Am J Crit Care. 2006;15:30-37.
Mike McEvoy, PhD, NRP, RN, CCRN, is the EMS coordinator for Saratoga County, New York, and the professional development coordinator for Clifton Park and Halfmoon Ambulance. He is a nurse clinician in the adult and pediatric cardiac surgery intensive care units at Albany Medical Center, where he also teaches critical care medicine. McEvoy is the chief medical officer and firefighter/paramedic for West Crescent Fire Department in Clifton, New York. He is also the chair of the EMS Section board of directors for the International Association of Fire Chiefs and a member of the New York State Governor’s EMS Advisory Council. He is a lead author of the textbook Critical Care Transport, the “Informed” Pocket References (Jones & Bartlett), and the American Academy of Pediatrics textbook Pediatric Education for Prehospital Professionals (PEPP).



Great job addressing these issues. Two things that can be problems are there are very few minutes worth of air on a small tank when using cpap and in the era of COVID many are afraid to use it because of pushing the virus around the back of the ambulance.