COPD Upgrade: What I Wish They Taught Me in Paramedic School
COPD patients don’t fit tidy categories. learn how inflammation, air trapping, and work of breathing actually guide care.

COPD patients don’t fit tidy categories. learn how inflammation, air trapping, and work of breathing actually guide care.

Follow a call that breaks down wheezing, pneumonia, and emphysema, using capnography to sharpen respiratory assessment skills.

Joseph Adelman outlines practical CPAP use in acute cardiogenic pulmonary edema and hypoxemic respiratory failure.
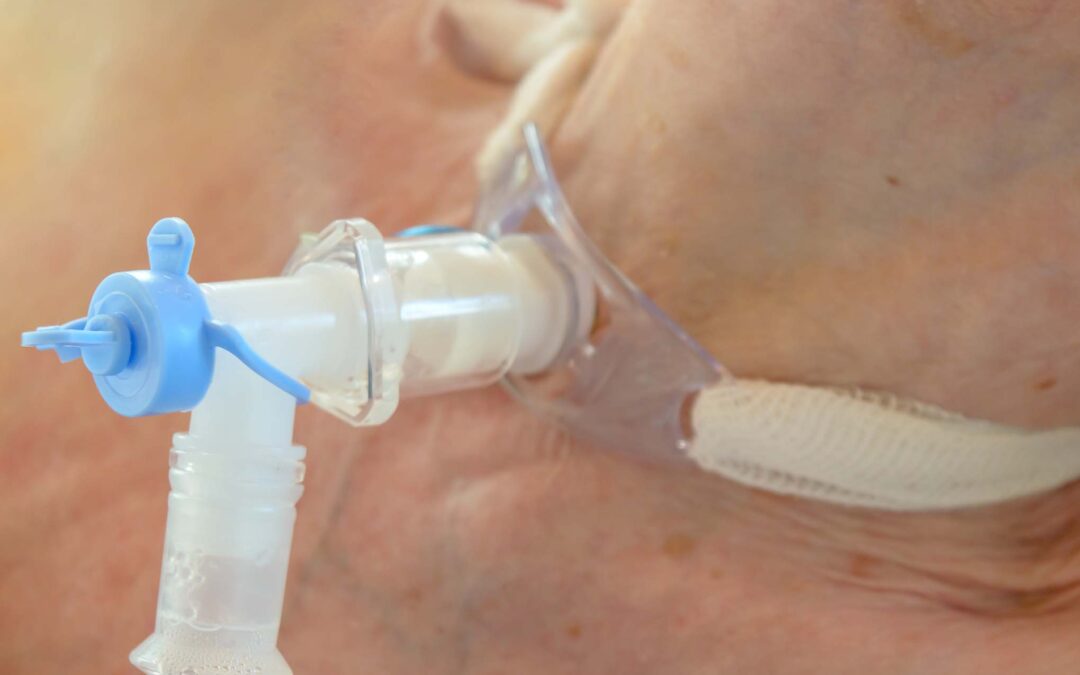
Learn how EMS providers can recognize, troubleshoot, and manage life‑threatening tracheostomy emergencies by having a clear, proactive plan.

Learn how proper airway ramping and ear‑to‑sternal‑notch positioning improves ventilation, reduces resistance, and enhances patient outcomes.

A ballistic missile from Iran struck Beersheba, Israel, prompting a medical response for 20 patients, including a critically ill 90-year-old woman.
Recent Comments