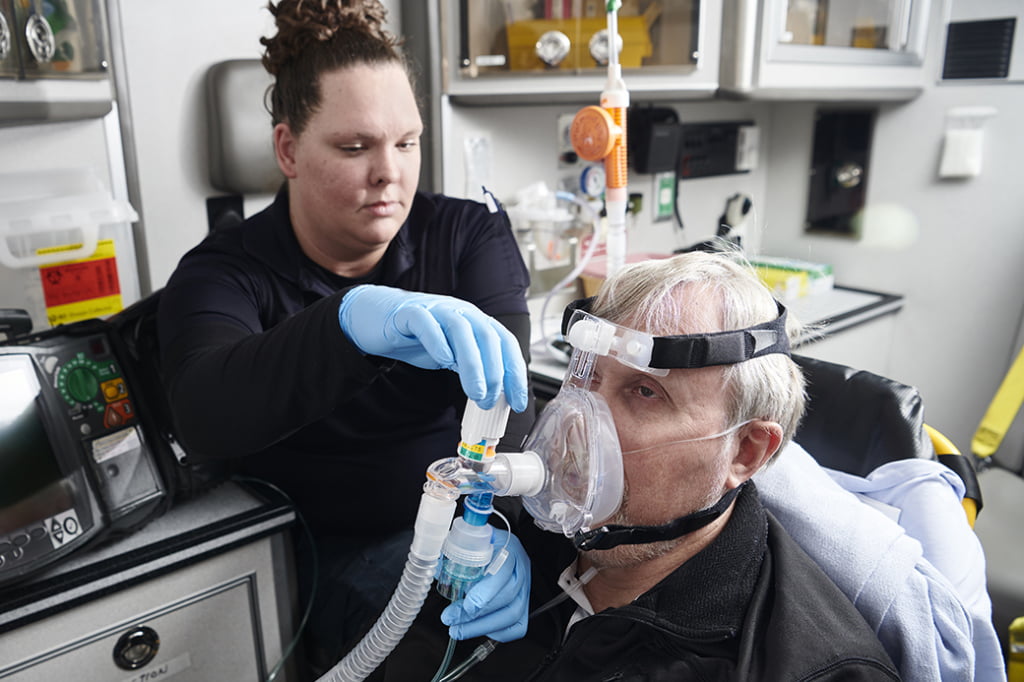
A typical treatment regime starts with a nebulized beta-agonist to relax the smooth muscle in the bronchi. (Photo/Pulmodyne)
You are dispatched to a difficulty breathing call at a soccer field 30 minutes away. On arrival, you see a small crowd of on-lookers gathered around your soon to be patient. Your initial assessment reveals a mid-twenties female in respiratory distress. Her respiratory rate is greater than 40 beats per minute (BPM), and the patient is seated, speaking in half sentences, and extending her arms on her knees to support her upper chest (tripod positioning). You notice a metered dose inhaler (MDI) in her right hand. She states she has taken eight puffs with no relief.
As your partner connects the monitor, you obtain some additional information from the patient. She was diagnosed with asthma at six years old and has been intubated once at age twelve for status asthmaticus. Your monitor is alarming high heart rate, with vital signs: HR 144, RR 42, BP 134/91 and SpO2 90% on room air. You listen to breath sounds and hear no movement in the bases with faint expiratory wheezes in the apices. The closest hospital is 35 minutes away.
Previous: Increasing Intubation First-Attempt Success Rates in Patients of All Ages
Your first plan of action is to place the patient on CPAP of 5 cmH2O and start an albuterol nebulizer while you load and go. As you apply the CPAP mask, the patient informs you she is claustrophobic and she appears increasingly anxious despite continual reassurance. Repeat vitals are: HR 148, RR 44, BP 141/93, and SpO2 98% and she is beginning to fail your “look” test. Do you have a backup plan?
Asthma, in the most simplistic definition, is a chronic disease of the airways. The more precise definition as described by the Global Initiative for Asthma is: “A heterogeneous disease, usually characterized by chronic airway inflammation… defined by the history of respiratory symptoms such as wheeze, shortness of breath, chest tightness, and cough that vary over time and in intensity, together with variable expiratory airflow limitation.”1 The term reactive airway disease (RAD) is often loosely used when asthma is not confirmed by diagnostic testing. Reactive airway disfunction syndrome (RADS), or irritant-induced asthma, refers to an airway disorder resulting from an intense exposure to an inhaled chemical irritant or noxious gas.2 It mimics asthma features such as airflow obstruction and bronchial hyperresponsiveness. In each of these, airflow obstruction is in fact the major concern.
Many of us are familiar with asthma and people who are able to control their asthma with minimal side effects and rare exacerbations. The U.S. Centers for Disease Control and Prevention report that one in 13 people have asthma.3 Ten Americans die from asthma each day, amounting to 3,564 deaths in 2017. Many of these deaths could have been avoided with proper treatment and care.4 The term “status asthmaticus’ is not well defined, and is used when a patient presents with an acute exacerbation of bronchial asthma that is not responsive to the usual treatment prescribed for asthma. Patients that present with status asthmaticus need prompt evaluation followed by aggressive therapy. This is where your experience and skills come into play.
Previous: Essentials of BiPAP
What you can and cannot administer is governed by your level of certification, and your state or local protocols. It is your responsibility to understand the policies and protocols that drive your decisions for care. There are no specific guidelines for the management of status asthmaticus, so patient education and targeted therapy are still the best means to manage asthma and minimize asthma attacks.
Let’s look further at the patient described above. How would you manage this patient’s care for the 35-minute ride to the hospital? A typical treatment regime starts with a nebulized beta-agonist to relax the smooth muscle in the bronchi. There are short-acting beta-agonists (SABAs) and long-acting beta agonists (LABAs). The effects of SABAs like albuterol, Proventil®, and levalbuterol may be evident within five to 10 minutes when administered properly, and last between three to six hours. We often add ipratropium bromide to albuterol (DuoNeb® or Combivent®) as ipratropium bromide is an anticholinergic bronchodilator that also helps dilate the airways. The LABAs are more for long term maintenance of asthma and chronic obstructive pulmonary disease (COPD) and typically contain an inhaled steroid to reduce inflammation.
CPAP is a good choice for the patient described above as the continuous positive airway pressure will help decrease the work of breathing and help stent the airways open. Corticosteroids would be the next medication to administer. Systemic corticosteroids given early in the course of treatment of acute asthma exacerbations have demonstrated overall effectiveness and are recommended by some asthma guidelines.5 Other strategies for this patient may be magnesium sulfate (MgSO4), a bronchodilator that may also increase the bronchodilator effects of β2-agonists by increasing their receptor affinity.6 Magnesium sulfate is typically given as a two gram IV bolus.
Another adjunct therapy to consider for the anxious patient with claustrophobia is low-dose ketamine. Ketamine may improve airway resistance and lung compliance with its positive bronchodilatory effects which will decrease the work of breathing. It might be beneficial to administer IM epinephrine at doses of 0.3 mg to 0.5 mg every 20 minutes for three doses. Terbutaline is another medication that can be considered if epinephrine is unavailable for the status asthmaticus patient that is headed towards intubation. Dosing for adults and pediatrics is 0.25 mg initially. If there is no significant improvement, a second dose of 0.25 mg administered can be administered in 15 to 30 minutes. Epinephrine shortages have pushed many EMS systems to substitute terbutaline. Nebulized epinephrine at IV doses are sometimes considered as a last-ditch effort for refractory status asthmaticus but their use has not shown to offer significant advantages over other therapies mentioned.7
A strategy usually reserved for the ED setting is Heliox, which is a specific mixture of oxygen and helium (80:20 or 70:30). Helium is a colorless, tasteless, non-combustible gas with a density seven times lighter than air. This lighter gas contributes to a more laminar (smoother) flow of air as opposed to the turbulent (chaotic) flow being created within the lungs. It is often misunderstood and under-utilized in the emergency setting.
If the patient’s condition is worsening, the obvious course would be to consider intubation for impending respiratory failure. This where you earn your money. To tube or not to tube, that is the question. The author has much experience with this conundrum and will often opt to exhaust all other options before resorting to mechanical ventilation. The challenges associated with oxygenating and mechanically ventilating a patient include barotrauma (pneumothorax) from the expected high pressures needed, patient synchrony with the ventilator and the hemodynamic effects resulting from such high pressures, and air-trapping/auto-peep from the airway obstruction present in acute asthma.
Asthma is a serious life-threating condition that can present benignly one minute and turn into respiratory failure in a heartbeat. Knowing the patient’s history and doing a thorough physical exam is your first priority when caring for this patient population. It is also imperative that you understand your local and state limitations for your scope of practice to provide the best quality of care for your patients.
References
- Global Initiative for Asthma. Global strategy for asthma management and prevention. ginasthma.org. [Accessed on June 13 2019].
- Christopher H Fanta, MD Asthma in adolescents and adults: Evaluation and diagnosis 1/29/2020.
- CDC.gov. (2019). CDC – Asthma. [online] Available at: https://www.cdc.gov/asthma/default.htm. [Accessed 13 June 2019].
- CDC.gov. (2018). CDC – Asthma – Most Recent Asthma Data. [online] Available at: https://www.cdc.gov/asthma/most_recent_data.htm. [Accessed 13 June 2019].
- A controlled trial of methylprednisolone in the emergency treatment of acute asthma. Littenberg B, Gluck EH N Engl J Med. 1986 Jan 16; 314(3):150-2.
- Classen HG, Jacob R, Schimatschek H. Interaction of magnesium with direct and indirect-acting sympathomimetic amines. Magnes Bull. 1987;9:80–87.
- Mull CC, Scarfone RJ, Ferri LR, Carlin T, Salvaggio C, Bechtel KA, Trephan MA, Rissman RL, Gracely EJ. A randomized trial of nebulized epinephrine vs albuterol in the emergency department treatment of bronchiolitis. Arch Pediatr Adolesc Med. 2004 Feb;158(2):113-8. doi: 10.1001/archpedi.158.2.113. PMID: 14757602.
Michael Schauf, RRT-NPS, has been a registered respiratory therapist at Albany Medical Center Hospital in New York since 1994. He covers all in-patient units, ICUs, the adult and pediatric Emergency Departments and is a member of the neonatal/pediatric transport team at this Level I Trauma and Level 3 NICU Center. Michael is the founder of Vent-Pro Training, teaching medics and nurses around the world how to manage mechanically ventilated patients during ground, rotor, and fixed-wing transports. He has been a flight respiratory therapist since 1998, currently working for AirMed and as a clinical education specialist for AMR. Michael authored the respiratory chapter of, “Critical Care Transport, 2nd edition,” published by Jones & Bartlett and is an adjunct instructor in the Respiratory Care Program at Hudson Valley Community College.


