EMS Airway Articles
Follow the latest articles, clinical reviews, case studies, and experts on EMS Airway.
Subscribe to get email alerts as new content is posted.
Articles

Between Breath and Breakdown: Recognizing and Managing Respiratory Distress Before It Fails
There is a narrow transition between respiratory distress and respiratory failure in prehospital care.
Select Article Type

To sustain life, we trust our training. But how do we remain centered?
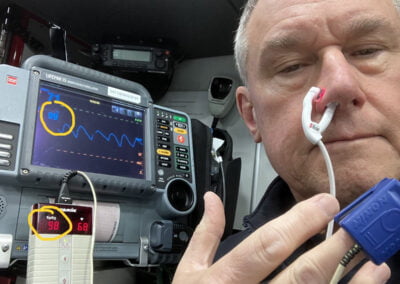
Here are some alternatives to the standard finger sensor for difficult SpO2 acquisition.
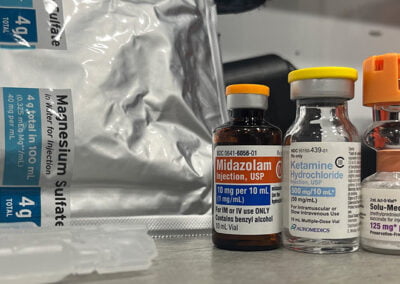
This is a case review involving a 25-year-old male patient presenting to EMS with respiratory failure secondary to status asthmaticus.
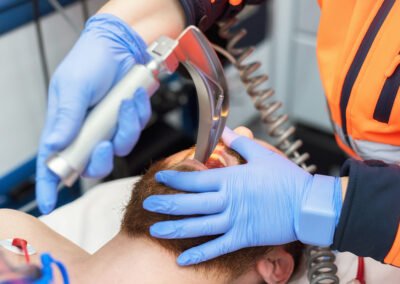
The author unpacks the utility of clinical bundles to address the dangers associated with airway management in a trauma patient.

This article delves into the critical components of cardiac arrest resuscitation during the prehospital phase.

An improper bag-ventilation technique may be the reason why a patient’s vital signs drop.
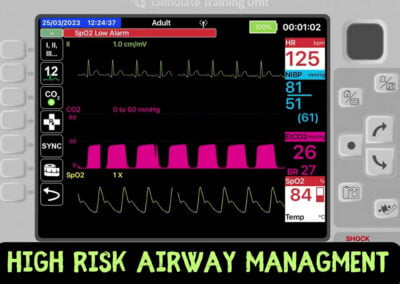
Here’s what you need to know about high-risk airway management.

This article emphasizes the importance of recognizing and managing the "physiologically difficult airway" in EMS.
Differentiating between pulmonary diseases is key in providing the correct and adequate treatment.
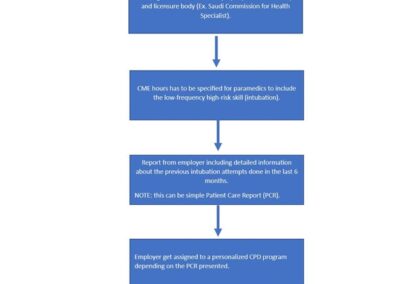
The authors propose creating a continuing professional development program for continuous monitoring and training of prehospital intubation skills.
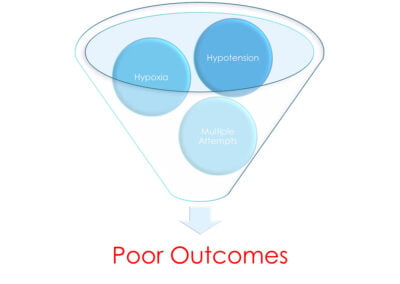
Research indicates hypoxia, hypotension and multiple intubation attempts in airway management greatly contribute to morbidity and mortality.
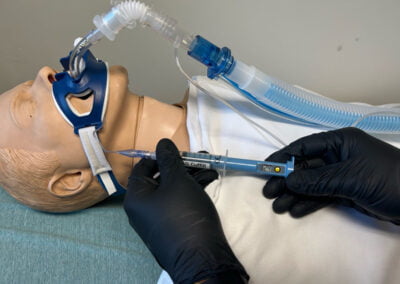
Inaccurate cuff pressure can lead to tracheal stenosis, ischemia and pressure ulcers, underlining the need for vigilant monitoring and adjustments.
JEMS Now Newsletter
Subscribe to JEMS and get the latest insights and information about the world of Emergency Medical Services directly to your inbox including the latest news, features and educational content on prehospital airway management.
